📊 Daily Data Brief: NEW❗️
As the dynamic and spread of the epidemic changes, I am adding a graph upfront. It shows the death growth curve of the epidemic (on a logarithmic case) for selected countries relative to a line showing doubling of death every 2.2 days (ECDC data and commentary here).
121,175 cases
New cases outside China: 4,371
New Cases in China: +34
% cumulative cases outside China: 33.3%
Total Death: 4,543 (+167)
Serious or Critical Cases: 5,748 (-23)
Source: https://www.worldometers.info/coronavirus/
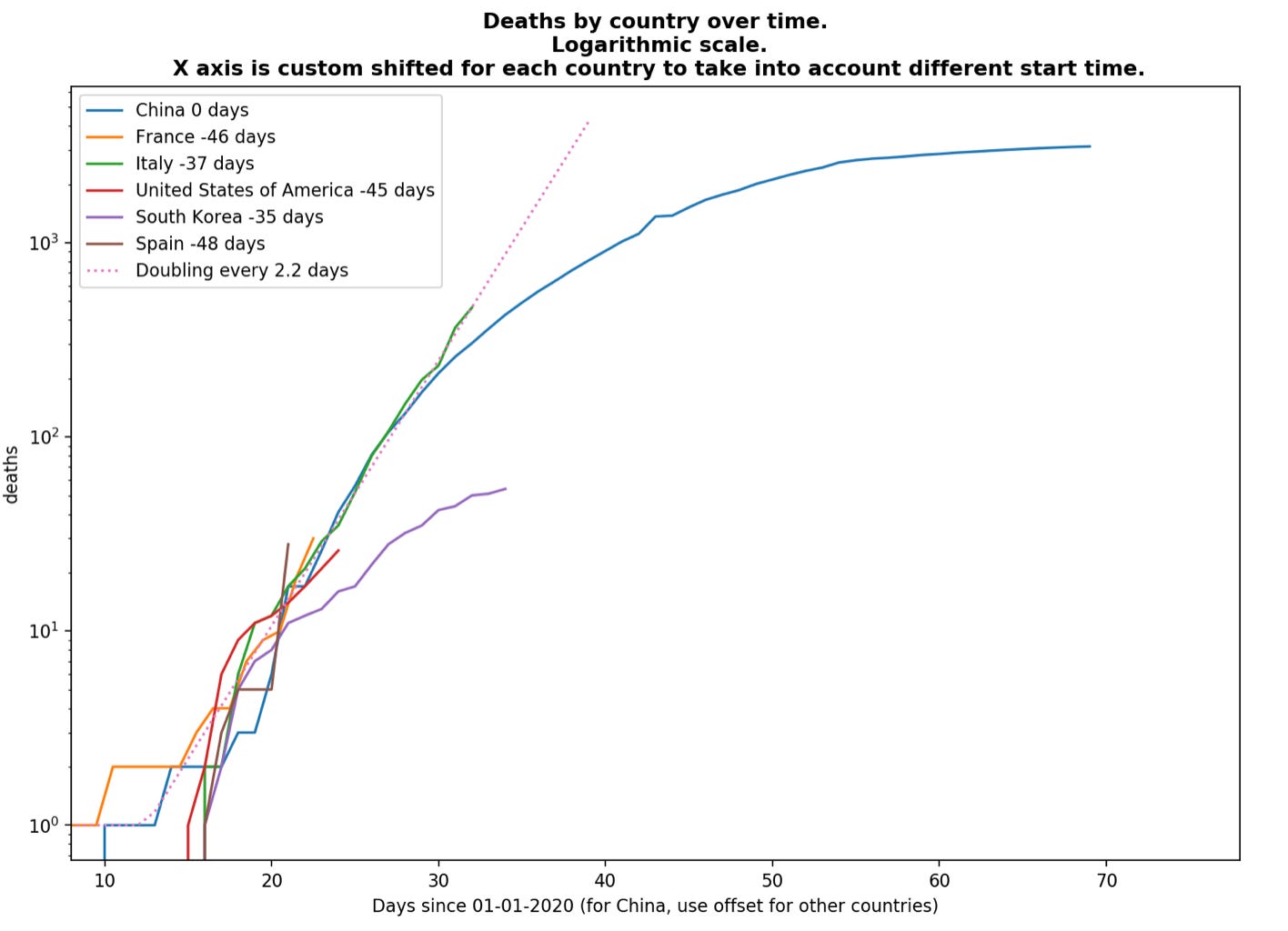
Cases have exploded in Italy and continue to grow exponentially (outside South Korea add China). Angela Merkel has announced that 60-70% of the German population will get COVID19 and the Chief Medical Officer in UK already pre-announced earlier in the week that a recommendation is forthcoming for British people who will have mild symptoms (expected to be around 80% of infected) to stay at home and isolate. All governments are now focusing on preparation for a severe epidemic, and on mitigation and increasing health capacity. Social distancing and behavioural change (wash you hands) remain key in slowing the spread of the epidemic and its ultimate severity, but the focus is also shifting on the next mitigation phase of our response. Testing will remain important in limiting the epidemic and testing capacity needs to continue increasing worldwide. However, officials have to balance the burden of testing in an exploding epidemic versus focusing their limited health capacity on care for hospitalised cases.
In my opening summary I also want to focus on “triage”. This is the definition in the Oxford Dictionary:
(in a hospital) the process of deciding how seriously ill or injured a person is, so that the most serious cases can be treated first
Triage has been with us in this epidemic for a while. It started by who gets to be tested in the US and elsewhere when testing ability is constrained (it is always the case with a new virus because developing a reliable test and scaling it is always a challenge). Triage will continue with who gets the ICU bed, the ECMO (Extracorporeal membrane oxygenation). As we get to that ICU triage stage the significance of it will dawn upon us. It will not stop there, it will continue when and if an effective vaccine becomes available a minimum of 12-18 months from now. Initially, like testing, production will be limited. Who will get it? For most of us who have not lived through a war (or catastrophe) we are becoming aware of a necessary a process which we have never experienced.
At the beginning we will most likely be looking at it from a personal point of view (will my parent get the ECMO?), but we should move quickly to think about the nurses and health workers who are faced with or make these decisions and question to what extent it needed to be that severe for them and the patients. There are obviously procedures and best practices put in place for the decision-making. They are inevitable to assist the healthcare professionals deal with the life-changing decisions that they will be making at scale in a constrained health system. It will however not shield them from the trauma they will inevitably be left with. In most countries we have accepted or witnessed a continuous cut on public health spending. We are bearing the consequences of it now with COVID19. A rethink will be needed. The upcoming and inevitable triage which is upon us will make us reflect on what we want for the future.
Today (if not already started) we need to change our individual and societal behaviour to ease the extent of triage: first social distancing (self-imposed or directed), washing your hands and soon staying at home if you can cope will mild symptoms. These timely societal steps at scale will make a huge difference on scale of triage and severity of the epidemic (see video below on exponential growth). Second, a debate will have to follow on public health spending when we come out of the current epidemic.
What happens to the virus and triage is still up to us.
🇮🇹 Video of the day: from the frontlines in Italy
This is a video from Giacomo Grasselli, a senior government official coordinating the network of Intensive Care Units (ICU) in Lombardy. He says that what has hit his region is “worse than a bomb” as unlike a bomb the intensity of the deflagration of the epidemic keeps increasing. He also talks about the necessity of triage which I discussed in my summary (Video Link)
🩺 Matthew K. Wynia and John L. Hick write a very important article In STAT news: “If Covid-19 gets bad, triage will be needed. Are we ready for that?”. It goes through the ethics of it and lessons learned from the past (including the H1N1 epidemic which in the US alone infected 60 million people, requiring 275,000 hospitalisations and causing 12,000 deaths between April 2009 and April 2010).
“So far, about 2% of people with diagnosed Covid-19 have died, and between 5% and 10% have required intensive care. But if even a small fraction of a very large number of infected people might benefit from critical care resources like mechanical ventilation or extra-corporeal membrane oxygenation to help them breathe, difficult triage decisions could be required.”
It is a sobering read (Link)
🧪 It is become apparent that COVID19 “is everywhere”. It is less in countries where testing capacity has not matched the speed at which this novel coronavirus spreads, and where the reported case numbers appears low (the US I am particularly looking at you). There is another article on the consequence of the US testing fiasco written in the New York Times. I believe it is more important to look now at where we are and what we can do to limit the severity of the epidemic rather than continue to lament on past mistakes for too long. All countries are ramping up their testing capacity now and that is what matters.
This is also what Marc Lipsitch explains in an excellent Twitter thread about the “absurdity” to now focus and dedicate resources on an exponentially gullible contact tracing effort rather than focusing primarily on social distancing to curb the rush of patients overwhelming healthcare capacity. He substantiates his thinking with an excellent research paper (“The Demand for Inpatient and ICU Beds for COVID-19 in the US: Lessons From Chinese Cities”) comparing early “social distancing” intervention in Guangzho (started at 7 confirmed cases and 0 death) versus Wuhan (495 confirmed cases and 23 death) and its impact on peak ICU demand. The data is clear: early intervention in “social distancing measures” makes a massive difference, particularly if we are unable (or unwilling) to enforce social distancing with the same authoritarianism as China. (Twitter thread Link)
❗️ As Coachella finally gets postponed “Cancel Everything” written by Yascha Mounk in the Atlantic narrates Marc Lipscitch fact-based recommendation above and advocates the same conclusion. School closures and other measures are coming. We should welcome them as good interventions. (Link)
📊 “Coronavirus: Why You Must Act Now” is a rather long read urging with data analysis from China, why government and business leaders must act now. Tomas Pueyo explains simply and with great visuals that however imperfect the data is we can infer pretty accurately the spike of the epidemic we are either witnessing now (Italy) or are a few days away from experiencing. A long but worthwhile read (Link)
❗️ Slightly more alarmist, but one wonders if that is what is needed to urge the needed public awareness and compel leaders into urgent action globally, Tom Frieden (President and CEO of Resolve to Save Lives) asks the question: “Could Coronavirus Kill a Million Americans?”. Frieden was the head of the CDC under Obama and was asked this exact question by Obama in June 2009 when H1N1 was hitting the US. This is what he writes:
I replied, with more certainty than I felt, “No, Mr. President, we won’t.” If asked the same question today about the novel coronavirus, I would have to reply, “I hope not, but that’s a possibility.”
He urges to plan for the worst, and like many today to implement immediately with resolve and discipline the measures which will “limit spread, improve survival and reduce the societal cost of COVID19” (Link)
💰 Moving on to the economic costs as more central banks cut interest rated (the Bank of England this morning) in spite of monetary policy not being as effective a tool as fiscal policy to combat the forthcoming COVID19 supply-side induced recession, Claire Cain Miller in the New York Times makes the case for bringing again a paid sick-leave bill in the US. Such bill has been stalled in congress since 2004 and has been reintroduced this week by the Democrat hoping that it will find bi-partisan support. President Trump said on Monday that he would announce worker relief measures yesterday but ended up missing in action. Let’s hope that the delay is because of the size and the comprehensiveness of the package rather than because he needs to cut it back to set aside aid for looming bankruptcy of the whole US shale gas industry following the 30% drop in oil prices on Monday. Such a possibility was reported by the Washington Post yesterday. (Link)
📊 A picture is worth a thousand words
Data and chart regularly updated by the Centre for the Mathematical Modelling of Infectious Diseases at the London School of Hygiene & Tropical Medicine. It maps the effective reproduction number (also known as R0) of COVID19. You want to get it below 1 as fast as possible to contain an epidemic. (Link to see charts and more data about your country)
This is a great COVID19 Dashboard prepared by Andrzej Leszkiewicz. Andrzej has also written an introductory and explanatory blog for it (“Coronavirus disease (COVID-19) fatality rate: WHO and media vs logic and mathematics”). It is a very extensive dashboard with 28 pages. I particularly like the country comparison tab, which allows you to track and benchmark the curve of the epidemic (number of cases and deaths) in your country with that of another. Very well done and informative. (Link)
Updated❗️(new narrative) This is a GitHub made by my friend Francois Lagunas (co-founder and CTO extraordinaire of Stupeflix, a company we backed). He has written a script to scrape deaths and number of cases in order to visualise the rate of growth on a logarithmic scale. He has taken a time offset for countries assuming that South Korea and Italy are 36 days behind China’s outbreak, and France and the USA a further 9 days behind. You can clearly see that South Korea is an outlier (as already shown in my newsletter “Better safe than sorry” and that the severity of this outbreak will depend on the behaviours of the governed and the decisive action of our respective governments. (Link)Singapore remains the gold standard of dashboard. Here is an article with the Best and Worst of all dashboard in the world, with Pros and Con prepared by Neel V. Patel for MIT Technology (Article)
This is the New York Times data and graph page on COVID19 with an update map of the US alone (Link)
🎬 One video and one podcast:
There is an excellent video explaining “exponential growth” and epidemics. Although we are all familiar with the phrase, its authors rightly says that “yet human intuition has a hard time recognising what it means”. This is a ❗️MUST WATCH❗️to understand fully what is upon us but also how early behavioural changes at scale can have a massive impact on the level of exponential growth of COVID19 (Link)
Dr Ashish Jha (director of the Harvard Global Health Institute) spoke with WBUR's All Things Considered host Lisa Mullins about what the numbers are telling him about hospital capacity in Massachusetts and the surge the state is about to experience:
"Some of the best epidemiologists in the world are estimating that between 40 and 70% of adults will end up getting an infection. Even if we begin with that low end of 40% of adults in Massachusetts, that's 2 million people getting infected. If we take data from China that says 20% of people needed hospitalizations, that's 400,000 hospitalizations. Even if we said 'No, that's too many, we can cut that in half,' that's 200,000 hospitalizations. At any given time in Massachusetts, we think there are [3,000 to] 4,000 hospital beds open at most ...
(Podcast Link)



Thank you for your excellent (daily) work.
Self-recommending, admittedly, but you might find this short piece on four complex system dynamics mechanics (exponential growth, phase changes, delayed feedback, leverage points) which mess with our intuitions interesting/relevant: https://medium.com/@dannybuerkli/gradually-then-suddenly-four-concepts-that-may-help-us-think-clearly-about-the-coronavirus-671e2583f828?source=friends_link&sk=981e3faf05a76f97ad2d3b0cdc18146b
Not that you need this explained to you but I‘ve seen a lot of people share it with their „this is all exaggerated“ friends to decent effect.